A Rare Case of Idiopathic Adult Intussusception
Anish D Thomas*, Mark Sayegh , Elisha Shah, Jina J Joseph and Mark Samarneh
DOI10.36648/2471-8041.21.7.191
Anish D Thomas1*, Mark Sayegh1, Elisha Shah3 , Jina J Joseph2 and Mark Samarneh1
1Department of Internal Medicine, St Johns Riverside Hospital, Yonkers, New York
2Department of Urology, Mount Sinai, New York
3Department of Internal Medicine, Lake Erie College of Osteopathic Medicine, New York
- *Corresponding Author:
- Anish D Thomas Department of Internal Medicine, St Johns Riverside Hospital, Yonkers, New York, Tel: +9145061326; E-mail: athomas4441@gmail.com
Received date: July 09, 2021; Accepted date: July 23, 2021; Published date: July 30, 2021
Citation: Thomas AD, Sayegh M, Shah E, Joseph JJ, Samarneh M (2021) A Rare Case of Idiopathic Adult Intussusception. Med Case Rep Vol.7 No.7.191
Abstract
Intussusception is rare in adults compared to children. Therefore, cases of adult intussusception are not well reported or easily recognized. Only 5% of all intussusception cases occur within the adult population and only 1% of all bowel obstruction pathology is due to the illness. They are most commonly found in male children, aged 6 months to 3 years old. Many childhood cases tend to be idiopathic, while in adult cases, malignant neoplasms are found to be the lead point at which the proximal segments get caught upon. Generalized abdomen pain is the most common symptom reported in adult due to peristalsis of the intestines occurring over the intussuscepted portion of the bowel. This case report focuses on a 34 year old female that presented with vague symptoms of nausea, vomiting, diarrhea, and abdominal pain. After obtaining extensive medical history, ruling out the common differentials, and obtaining imaging of the abdomen, idiopathic jejunal intussusception is found to be the diagnosis in this patient. The patient was treated conservatively with antibiotics and pain management. The intussusception self-resolved and the patient was discharged home.
Introduction
Intussusception occurs when the proximal portion of the bowel (intussusceptum) slides into the distal portion of the small or large bowel (intussuscepiens) [1]. This “telescoping” prevents food and fluid from passing forward and cuts circulation to the part of the intestine affected [2,3]. Intussusception can be life threatening because the telescoping causes obstruction and leads to proximal bowel distension; this increases intraluminal pressure causing micro vascular ischemia, tissue necrosis, and, potentially, intestinal perforation and peritonitis [3]. Children classically present with the triad of colicky abdominal pain, currant jelly stools, and sausage shaped abdominal mass. Conversely, adult patients present with diffuse abdominal pain, nausea, vomiting, bloody stools, change in bowel movements, or abdominal distension[3]. The diagnosis is difficult to initially recognize in adults due to symptoms being similar to other gastrointestinal diseases such as Crohn’s disease, bowel obstruction, gastroenteritis, pancreatitis, diverticulosis [3,4].
Case Presentation
This case report involves a 34 year old female with a past medical history of Helicobacter pylori infection and an abnormal Papanicolaou smear, who presented to the emergency department with nausea, vomiting, diarrhea and abdominal pain of 24 hour duration. She reports nausea, multiple episodes of non-bilious vomiting, and loose watery stools. She does not recall eating anything out of the ordinary and denies any sick contacts or travel. She reports attributing her symptoms initially to her current menstrual cycle. She also noted unintentional fluctuations in her weight, but no loss of appetite. Her vitals were stable upon arrival and during the course of her stay at the hospital. She denies cigarette use but does admit to marijuana use. She had generalized abdominal pain with greater emphasis in the lower quadrants. The patient notes a long standing history of chronic abdominal pain with nausea, vomiting, and diarrhea. She had an esophagogastroduodenoscopy seven months prior for iron deficiency anemia which showed gastritis and a Helicobacter pylori infection, which was then subsequently treated. She underwent a colonoscopy in 2019 for colitis with pathology report showing chronic lymphocytic microscopic colitis, which was managed conservatively. She confirms no family history of colorectal cancer or irritable bowel disease. Further work up included CAT scan, stool study, and upper gastrointestinal series with small bowel follow through.
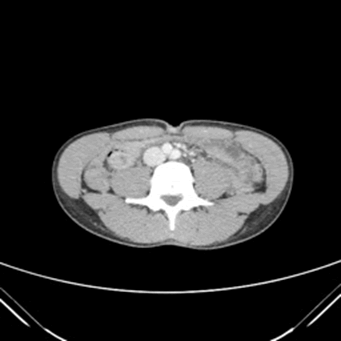
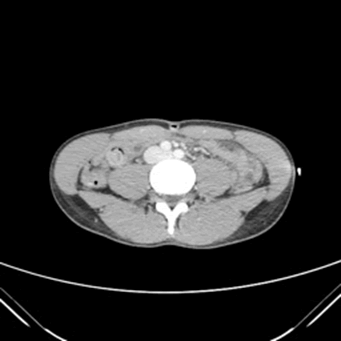
The CAT scan reported nonobstructive jejunojejunal small bowel intussusception in the right paramedian aspect of mid to lower abdomen over a length of three centimeters (Figure 1). Thereafter, the patient was treated medically with symptomatic management and antibiotics including ciprofloxacin, metronidazole, and piperacillin/tazobactam. A nasogastric tube was inserted, and 150 mL of dark green drainage was suctioned out. No surgical intervention was required, and the intussusception resolved on its own, as exhibited on the repeat CAT scan (Figure 2). Outpatient gastrointestinal follow up was suggested to the patient to monitor for recurrence.
`
Discussion
Cases of adult intussusception are uncommon; therefore, it is often missed and rarely reported. Patients come in with symptoms similar to other gastrointestinal diseases, making diagnosis difficult. In most cases, there is a lead point upon which the intussusception occurs; 60% of colonic and 30% of small bowel intussusception are due to a malignant tumor, while only 10% of small bowel intussusceptions are idiopathic. Because of the high likelihood of malignancy, when intussusception is presumed, patients undergo a CAT scan of the abdomen, rather than an ultrasound, as would be done in pediatric cases. The CAT scan is useful in locating the intussusception as well as any lead points. If an ultrasound of the abdomen is done, the classic signs are similar to those found in pediatric patients, which includes the “target” and “pseudokidney” signs [5,6]. In this case, the patient underwent a CAT scan of the abdomen, which showed a jejunojejunal intussusception with no signs of malignancy. The treatment of choice in most adult patients with intussusception is surgical resection of the malignancy and any infarcted portion of bowel rather than reduction with hydrostatic enemas as done with pediatric patients. Preoperative reduction in adult cases increases the risk of perforation or seeding of cancerous or infectious cells; this procedure also increases the risk of surgical complications due to manipulation of a friable and edematous bowel [1]. Because it is difficult to distinguish malignant from benign lead points, manual reduction should not be done unless there is a direct confirmation of what the lesion is, either by endoscopy or surgery [1]. For some patients, in whom malignancy has been definitively ruled out and has presumed idiopathic intussusception, a trial of symptomatic treatment can be attempted with antiemetics, antibiotics, and pain relief. Avoiding unnecessary resection in benign causes of intussusception prevents short gut syndrome, which involves a portion of the bowel to be taken out preventing proper absorption of water and nutrients; this can result in failure to thrive in infants and severe malnutrition in adults. In this case, the patient was not found to have a definitive cause and therefore, was treated with pain medications, antiemetics, and antibiotics and the intussusception self-resolved within 2 days of admission.
This patient’s specific presentation led to the diagnosis of idiopathic intussusception due to several factors. She came in with vague gastrointestinal symptoms of nausea, vomiting, and diarrhea that occurred abruptly. A thorough investigation with comprehensive history taking, imaging, and prior colonoscopy results, no pathological lead points were identified, including the most common, malignancy. After ruling out more common causes of abdominal pain, and considering CAT scan findings, idiopathic jejuno-jejunal intussusception was concluded as the diagnosis. Therefore, the patient underwent symptomatic management and was discharged home.
Conclusion
Adult intussusception is a rare condition that can progress to complications in certain cases, including, bowel ischemia or perforation. Due to the infrequency of the cases, evidence for classic signs and symptoms are less obvious; therefore, diagnosis tends to be late. This case report helps to raise awareness of this rare clinical phenomenon observed in adults. Therefore, it will aid physicians in recognizing and identifying intussusception as part of the differential diagnosis for patients who come in with classic gastrointestinal symptoms. Early recognition and intervention can help prevent complications that can arise from misdiagnosis or late diagnosis.
List of Abbreviations
CAT scan: Computed Tomography
Acknowledgement
The authors have provided the support for Conceptualization, Validation, Original draft preparation, Review & Editing, Visualization, Supervision, Investigation, Resources, Project administration.
Conflict of Interest
The authors have no conflicts of interest to disclose and had access to all data pertaining to the case when writing this manuscript.
References
- Toh Yoon EW (2016) Treatment of adult idiopathic ileocolic intussusception with non-operative reduction under fluoroscopic guidance. Gastroenterol Hepatol Endosc.
- Intussusception. (1998-2021). Mayo Clinic. 6, 2021.
- Hadid T, Elazzamy H, Kafri Z (2020) Bowel Intussusception in Adults: Think Cancer!. Case Rep Gastroenterol 14:27-33.
- Aref H, Nawawi A, Altaf A (2015) Transient small bowel intussusception in an adult: Case report with intraoperative video and literature review. BMC Surg.15: 36
- Eze VN (2016) Idiopathic intussusception in an adult an image guided diagnosis. BJR Case Rep. 2(2):20150508.
- Lu T, Chng YM (2015) Adult intussusception. Perm J.19 (1):79-81.

Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences