Patient with Dactylitis and Enthensopathy- Forestier Disease - RADISH Variant
Luis Arturo Gutiérrez-Gonzalez and Salvador Malave
DOI10.21767/2471-8041.S1-007
Luis Arturo Gutiérrez-Gonzalez1* and Salvador Malave2
1Rheumatology and Internal Medicine Unit, El-Avila Clinic, Altamira, Caracas 1060, Venezuela
2Department of Radiology, Doximity, The Professional Network for Clinicians, Miami, Florida, USA
- *Corresponding Author:
- Luis Arturo Gutiérrez-Gonzalez
Rheumatologist, Rheumatology and Internal Medicine Unit
El-Avila Clinic, Altamira, Caracas 1060, Venezuela
Tel: +58212276.1582
Fax: +58212276.12583
E-mail: Umircaracas@yahoo.es
Received Date: Janurary 23, 2018; Accepted Date: Janurary 29, 2018; Published Date: January 31, 2018
Citation: Gutiérrez-Gonzale LA, Malave S (2018) Patient with Dactylitis and Enthensopathy - Forestier Disease - RADISH Variant. Med Case Rep Vol.4 No. S1:007. DOI: 10.21767/2471-8041.S1-007
Abstract
Diffuse idiopathic skeletal hyperostosis (DISH) is a bony hardening (calcification) of ligaments in areas where they attach to your spine. Also known as Forestier's disease, diffuse idiopathic skeletal hyperostosis may cause no symptoms and require no treatment. The most common symptoms are mild to moderate pain and stiffness in your upper back. DISH can also affect your neck and lower back. Some people have DISH in other areas, such as shoulders, elbows, knees and heels. A non-inflammatory condition, DISH can be progressive. As it worsens, it can cause serious complications.
This is a case report of a patient with dactylitis and enthensopathy - Forestier disease - RADISH variant
Keywords
Diffuse Idiopathic Skeletal Hyperostosis (DISH); Spondyloarthritis; Rheumatoid arthritis; Spinal symptomatology
Introduction
Diffuse Idiopathic Skeletal Hyperostosis (DISH) or Forestier’s disease is a condition whose primary manifestation is the ossification of the anterior longitudinal ligament (ALL) and the development of intervertebral bony bridges. Diffuse Idiopathic Skeletal Hyperostosis (DISH), also called Forestier’s disease is a rheumatological condition mostly affecting the axial skeleton. However, a subset of these patients presents with peripheral arthritis and enthensopathies that mimic spondyloarthritis and even rheumatoid arthritis. This group of patients is called RADISH (Rheumatism articular in Diffuse Idiopathic Skeletal Hyperostosis), a systemic disease characterized by bone neoformation in the ligament, tendon and capsular attachments.
Case Presentation
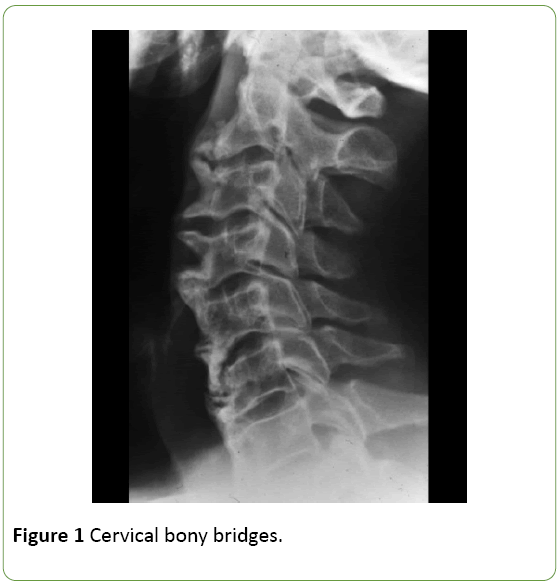
This is a 75-year old male patient presenting with a 10-year history of axial pain and mixed characteristics. The pain improves through the morning (<2 hours), and then gets better after resting at the end of the afternoon – evening [1,2]. The patient self-medicates with standard painkillers such as acetaminophen 1 gram, alternating with various NSAIDs (sodium diclofenac, ibuprofen and naproxen) using on demand dosing. Since the pain fails to improve and the patient experienced limited neck rotation, the patient decides to visit the rheumatologist. A complete Spine X-ray is required which upon studying the cervical spine evidences diffuse hyperostosis along the anterior aspect of the cervical spine, with bony bridges at various levels. The hyperostotic bone is present at the edges of the cortex of the original vertebral body at >45° angles; the intervertebral disc spaces are intact and there are no erosions or romanus sign (Figure 1).
A routine lab test in addition to an immune-rheumatological profile (ANA, Ra Test, Anti CCP and HLA B27) were requested, which were reported negative or within normal, and the patient was prescribed meloxicam 15 mg per day for 6 weeks, together with physical therapy resulting in satisfactory improvement [3,4].
14 months later the patient comes back presenting with boxing glove arthritis in the right hand only, in addition to arthralgia in both shoulders and ankles, with dactylitis of the 3rd left foot toe. A routine lab test was prescribed (CBC, blood chemistry, PPD (Tuberculin), feet X-rays, X-rays of both hands, Chest X-ray [5,6]. A recommendation was given to repeat the Ra Test and Anti CCP, just reporting elevation of acute phase reactants (VSG 78 mm; PCR 4,32 mg/dl) [7]. An ultrasound of the joints in both hands showed inflammation of all the tendon sheaths of the extensors of the fingers, with no erosions but just osteodegenerative changes consistent with age, but with a power/Doppler (+) sign. The patient started with deflazacort at a 30mg dose tapering by 6mg/week until a minimum dose of 6mg was reached, which was maintained for 3 months, with good response and tolerance [8].
Discussion
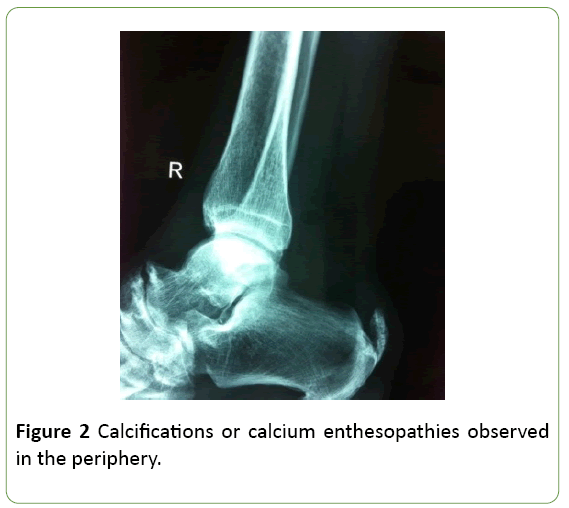
In the classical DISH the basic lesion is the ossification of the anterior longitudinal ligament (ALL) developing intervertebral bridges. Forestier and Rotès-Quérol in 1950 described the disease and called it ankylosing hyperostosis of the spine, as opposed to disc arthrosis or ankylosing spondyloarthritis. Resnick in 1975 recommended the term diffuse idiopathic skeletal hyperostosis, insisting on its systemic nature with extra-vertebral involvement and defined the specific radiological criteria currently used [9,10]. This pathology has been described in routine autopsies and presents more often in males between sixty and seventy years old. The spinal symptomatology is the most frequently described clinic, with pain, cervical and dorsal stiffness, but most of the patients are asymptomatic (Figure 2).
A DISH peripheral variant has been described called RADISH (Rheumatoid arthritis in diffuse idiopathic skeletal hyperostosis), where the patient presents with arthralgias and in some cases arthritis of the small and large joints that mimic rheumatoid arthritis, except for the absence of Ra Test and other biomarkers. From the clinical point of view, the age of presentation is mostly between 60 and 70 years old and is usually asymmetrical [11,12].
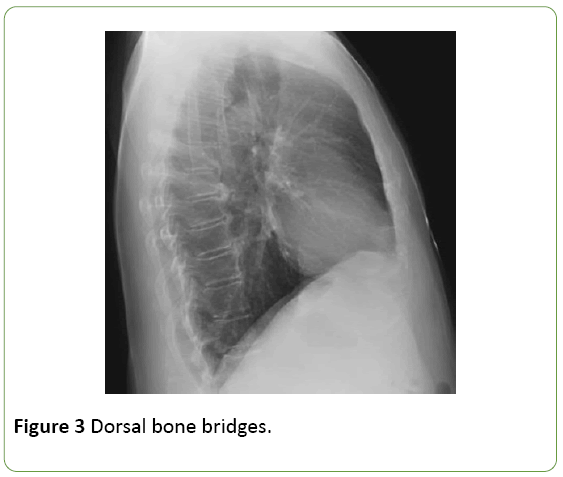
Among other radiological findings, RADISH differs from rheumatoid arthritis (RA) because usually osteoporosis is absent, but there is often bone sclerosis and proliferation of erosions, in addition to osteophytes and bone ankyloses. Some of the atypical clinical characteristics include a high incidence of flexion contractures of the elbows, wrists, ankles and knees. It is no surprise that the production of bone takes place on the joints involved in patients with RA-DISH, since the latter disorder is characterized by bone proliferation at the bone attachment sites of ligaments and tendons in the axial and extra-axial skeleton, probably stress related. One of the extraaxial manifestations of RA-DISH is dactylitis (Figure 3).
Criteria according to Resnick:
1. Presence of ossification along the anterolateral aspect of four contiguous vertebral bodies leading to the formation of bone bridges.
2. The relative preservation of the intervertebral disc height in the affected region and the absence of evolving radiological changes, hence confirming degenerative disc pathology.
3. The lack of erosion, sclerosis or bone ankyloses of the sacroiliac joints or the posterior interapophyseal joints.
Da ctylitis is a typical manifestation of spondyloarthropaties and in particular of psoriatic arthritis, though there are other causes that may cause this peculiar inflammation. There are inflammatory dactylitis (spondiloarthropaties, gout or sarcoidosis), infectious dactylitis (tuberculosis, syphilis or blistering distal dactylitis) or noninflammatory dactilitis (sickle cell anemia) [13,14].
Conclusion
Using conventional radiology, no vascular infarction of the bone marrow was identified in our patient, which is the typical lesion in sickle cell anemia dactylitis; even the blood test only reported VSG and PCR elevation [15]. In case of infection secondary to syphilis or brucellosis, no radiological signs of osteomyelitis were observed which the result of soft tissue damage is. There was no disruption either of the fat pad of the volar surface of the fingers (typical radiological lesion secondary to beta-hemolytic Streptococcus Group A infection) [16,17]. The only finding in our patient was a Tenosynovitis of the flexor sheath, typical of non-infectious inflammatory dactylitis and not due to crystal deposits or granulomatous tenosynovitis.
References
- Resnick D (1978) Radiographic abnormalities of rheumatoid arthritis in patients with diffuse idiopathic skeletal hyperostosis. Arthritis Rheum 21: 1-5.
- Morlock G (1993) Hyperostosevertébraleankylosante. EncyclMédChirAppareillocomoteur 15: 861.
- Forestier J, Rotès-Quérol J (1950) Hyperostoseankylosantevertébralesénile. Rev Rheum Dis 9: 321-330.
- McGonagle D, Gibbon W, Emery P (1998) Classification of inflammatory arthritis by enthesitis. Lancet 352: 1137-1140.
- Healy PJ, Helliwell PS (2007) Measuring dactylitis in clinical trials: Which is the best instrument to use? J Rheumatol34: 1302-1306.
- McGonagle D, Marzo-Ortega H, Benjamin M, Emery P (2003) Report on the Second International Enthesitis Workshop. Arthritis Rheum 48: 896-905.
- Olivieri I, Favaro I, Pierro A, Frisoni M, Ferri S, et al. (1994) Dactylitis also involving the synovial sheaths in the palm of the hand. Ann Rheum Dis 53: 783-784.
- Rothschild BM, Pingitore G, Eaton M (1998) Dactylitis: Implications for clinical practice. Semin Arthritis Rheum 28: 41-47.
- Olivieri I, Scarano E, Padula A, Giasi V, Priolo F (2006) Dactylitis, a term for different digit diseases. Scand J Rheumatol 35: 333-340
- Torralba KD, Quismorio Jr. FP, Brazille P, Timsit MA, Quillard A, et al. (1998) Tuberculousdactylitis in a single phalanx. Rev RhumEngl Ed 65: 511-512.
- Feldman F, Auerbach R, Jonson A (1971) Tuberculousdactykitis in the adult. Am J Roentgenol Radium TherNucl Med 112: 460-479.
- Zemtson A, Veitschegger M, Gelman MI, Everts CS (1973) Blastomycoticdactylitis. Radiology 107: 331-332.
- Haggard ME (1961) Sickle-cell anemia in the first two years of life. J Pediatr 58: 785-790.
- Almeida A, Roberts I (2005) Bone involvement in sickle cell disease. Br J Haematol 129: 482-490.
- Zemtsov A, Veitschegger M (1992) Staphylococcus aureus-induced blistering distal dactylitis in an adult immunosuppressed patient. J Am AcadDermatol 26: 784-785.
- Torralba KD, Quismorio FP. (2003) Sarcoidartritis: A review of clinical features, pathology and therapy. SarcoidosisVasc Diffuse Lung Dis 20: 95-103.
- Pitt P, Hamilton EB, Innes EH, Morley KD, Monk BE, et al. (1983) Sarcoiddactylitis. Ann Rheum Dis 42: 634-639.

Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences