A Case Report of Uncommon Presentation of Primary Pulmonary Epitheliod Haemangioendothelioma
Nik Nuratiqah Nik Abeed, Ummi Nadira, Effa Faieyzah and Andrea Ban Yu Lin
Nik Nuratiqah Nik Abeed1*, Ummi Nadira2, Effa Faieyzah3 and Andrea Ban Yu Lin4
1Medical Department, Universiti Kebangsaan, Malaysia
2Respiratory Unit, Universiti Putra Malaysia
3Histopathology Department, Universiti Kebangsaan, Malaysia
4Respiratory Unit, Universiti Kebangsaan, Malaysia
- *Corresponding Author:
- Nik Nuratiqah Nik Abeed
Medical Department, Universiti Kebangsaan, Malaysia
Tel: + 603-9145 7480
E-mail: kenix_atiqah@yahoo.com
Received date: April 19, 2019; Accepted date: May 13, 2019; Published date: May 16, 2019
Citation: Abeed NNN, Nadira U, Faieyzah E, Lin ABY (2019) A Case Report of Uncommon Presentation of Primary Pulmonary Epitheliod Haemangioendothelioma. Med Case Rep Vol.5 No.2:99.
Abstract
Pulmonary epitheliod hemangioendothelioma (PEH) is a rare tumour of endothelial origin with an intermediate course between hemangioma and conventional angiosarcoma. Hemangioendotheliomas are a family of vascular neoplasms of intermediate malignancy. It commonly occurs in woman with asymptomatic and the radiographic findings usually multiple bilateral small pulmonary lesions.
Keywords
Pulmonary epitheliod hemangioendothelioma; Tumour; Pulmonary lesions; Lung biopsy
Introduction
We reported a case of elderly man presented with clinical symptoms of prolong cough with radiologically findings of large solitary lung mass in Computed Tomography (CT) of Thorax with histopathologically and immunohistochemically proven as PEH. This patient undergone palliative radiotherapy and was planned for surgical intervention [1-3].
Case Presentation
We report a case of PEH in a 59 year, ex-chronic smoker gentleman, with underlying Diabetes Mellitus presented with a complain of on and off productive cough and dyspnoea for 1 year duration and was diagnosed to have Chronic Obstructive Pulmonary Disease (COPD) after done a lung function test and was started treatment of COPD with combination Fluticasone/ salmeterol accuhaler 50/500 mcg 2 puff twice a day. He had few admissions due to acute exacerbations with chest infections admitted treated with short course antibiotics and had loss weight 3 kg in one month durations after presented to the clinics for followed up. We investigated him for Pulmonary Tuberculosis however all results were negative.
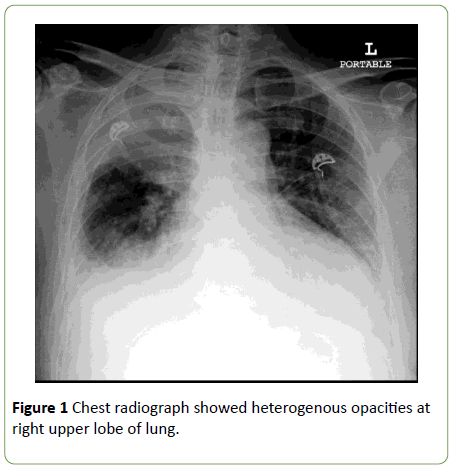
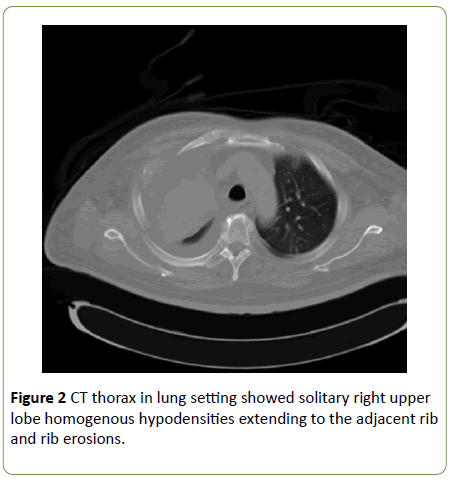
Chest radiograph demonstrated the right middle zone homogenous opacities with bilateral pleural effusion and noted the trachea deviate to the right which suggested lung collapsed and consolidation at the same time (Figure 1). However, repeated chest radiograph in 1 month post antibiotics treatment revealed the lesions remains, hence CT thorax was commenced and revealed right upper lobe heterogeneous enhancing mass with foci of calcification, adjacent 3rd rib erosion, presence of soft tissue pleural nodule with right axillary and mediastinal lymphadenopathy (Figure 2).
Bronchoscopy was performed and noted total occlusion of right upper lobe segmental bronchus by external compression with increased vascularity and contact bleeding at the area. Right upper lobe endobronchial tissue was send and histopathology findings consistent with hemangioendothelioma which microscopically showed underlying stroma harbours tumour cells forming small intracellular lumen and vascular spaces lined by mildly atypical endothelial cells. Immunohistochemically, the neoplastic cells are positive for endothelial markers CD31, CD34 and factor VIII.
He was referred to cardiothoracic surgical intervention and planned for Positron Emission- Computed Tomography (PET/CT) and CT thorax 3D reconstruction before proceed with surgical removal. Oncology team also reviewed the patient and the palliative radiotherapy was opted as the advanced disease if surgically unfit.
Discussion
Pulmonary epithelioid hemangioendothelioma (PEH) is a rare tumour of the lung [1]. Previously, it was first described by Dail and Liebow in 1975 as a variant of bronchial alveolar carcinoma called Intravascular Bronchioalveolar Tumour and subsequently the name changed as suggested by Weiss et al. as the development of immunohistochemical technique confirmed the tumour are from the endothelial lineage [4].
PEH can arise from many organs such as pulmonary, bone and soft tissues but the most frequent visceral affection is hepatic and the pulmonary localization remains rare. About 120 cases reported in the literature concluded that this tumour occurred in young age group with woman predominance and most of the patients are asymptomatic [5]. Different presentation with this case, patient is elderly man who is ex-smoker presented with dry cough for 1 year and constitutional symptoms and had mistakenly diagnosed COPD but eventually had endo bronchial obstruction due to external compression of the mass.
The most characteristic PEH on chest radiograph usually multiple pulmonary nodules with well or ill-defined margins ranging in size up to 2 cm in 20% cases in both lungs but 10% of the cases can be isolated pulmonary mass of less than 5 cm [6].
The pivotal diagnostic criteria are based on pathological findings and immunohistochemical analysis by obtaining the lung biopsy [7]. From literature, bronchial biopsy and bronchioalveolar lavage are not contributory, different from this case, the biopsy were from endobronchial area. Microscopically featured mononucleated cells of large sizes and abundant eosinophilic cytoplasm. The immunohistochemical staining for endothelial cell markers confirms PEH are antibodies anti CD31, anti-factor VIII and anti CD34 which all of these are positive in our case. FLI-1 is the most specific immune marker of PEH but it was not done in our center [7].
Prognosis of PEH is unpredictable. Previous case report showed that the prognosis based on clinical manifestation at presentation of PEH. In symptomatic young age with multiple bilateral pulmonary nodules or pleural effusion and mass more than 3 cm and high mitotic activity as well as cytonuclear atypicality, the prognosis is poor. Common complications are respiratory failure as a result of increasing size and number of lung nodules [8,9].
Conclusion
There is no standard treatment for PEH. The most common treatment is tumour resection. There are insufficient data to recommend a specific drug regimen although several chemotherapeutic agents have been tried. One case reported complete remission in those received carboplatin and etoposide. Some cases had benefit with bevacizumab, a monoclonal antibody that blocks VEGF-A. In conclusion, a suspicion of PEH should be borne in mind when presented with unusual presentation of the mass in the radiographic findings.
References
- Rosengarten D, Kramer MR, Amir G, Fuks L, Berkman N (2011) Pulmonary epithelioid hemangioendothelioma. Isr Med Assoc J 13: 676.
- Erasmus JJ, McAdams HP, Carraway MS (1997) A 63-year-old woman with weight loss and multiple lung nodules. Chest 111: 236-238.
- Leleu O, Lenglet F, Clarot C, Kleinmann P, Jounieaux V (2010) Pulmonary epithelioid haemangioendothelioma: reports of three cases and a review of the literature. Rev Mal Respir 27: 778-783.
- Dail DH, Liebow AA, Gmelich JT, Friedman PJ, Miyai K, et al. (1983) Intravascular, bronchiolar, and alveolar tumor of the lung (IVBAT): An analysis of twenty cases of a peculiar sclerosing endothelial tumor. Cancer 51: 452-464.
- Geramizadeh B, Ziyaian B, Dehghani M, Tahmasebi K (2014) Prolonged hemoptysis caused by primary pulmonary epithelioid hemangioendothelioma; a case report and review of the literature. Iran J Med Sci 39: 223.
- Bagan P, Hassan M, Barthes FL, Peyrard S, Souilamas R, et al. (2006) Prognostic factors and surgical indications of pulmonary epithelioid hemangioendothelioma: a review of the literature. Ann Thorac Surg 82: 2010-2013.
- Shao J, Zhang J (2014) Clinico-pathological characteristics of pulmonary epithelioid hemangioendothelioma: A report of four cases and review of the literature. Oncol Lett 8: 2517-2522.
- Ohopj NP, Yousem SA, Sonmez-Alpan E, Colby TV (1991) Estrogen and progesterone receptors in lymphangioleiomyomatosis, epithelioid hemangioendothelioma, and sclerosing hemangioma of the lung. Am J Clin Pathol 96: 529-535.
- Kim YH, Mishima M, Miyagawa-Hayashino A (2010) Treatment of pulmonary epithelioid hemangioendothelioma with bevacizumab. J Thorac Oncol 5: 1107-1108.

Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences